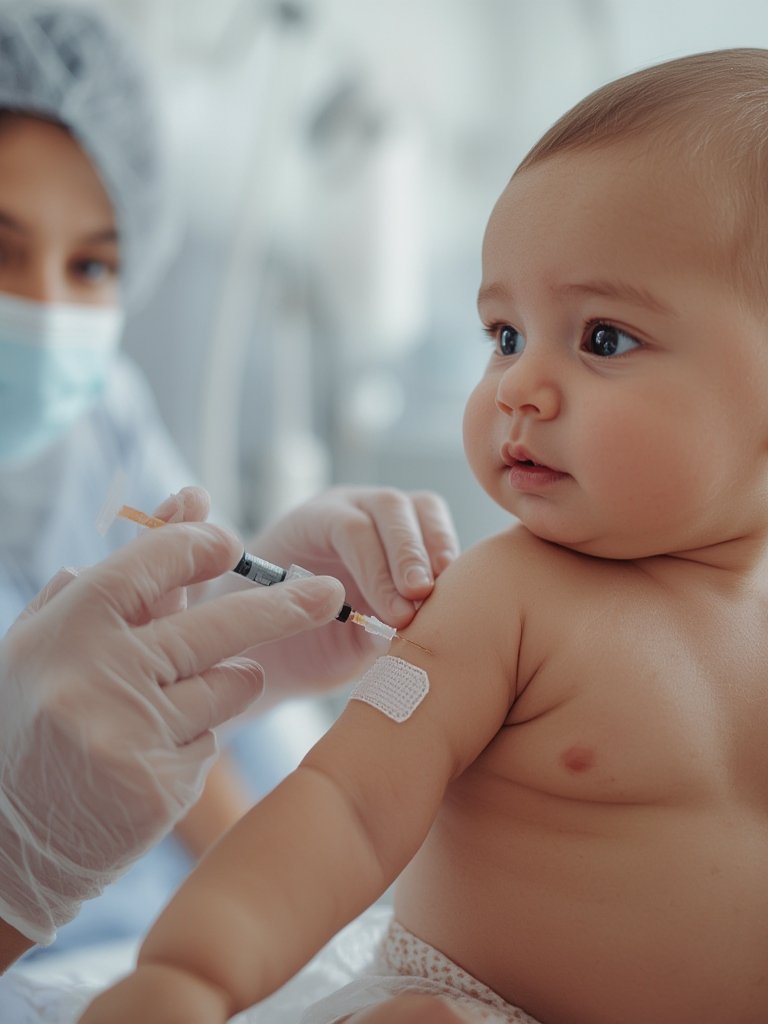
Baby vaccination schedule changes can directly affect every parent making health decisions for their baby. Whether you follow the CDC, WHO, or NHS, understanding the most current recommendations and overcoming real-world challenges makes all the difference for your child’s health.
Key Takeaways
- The U.S. baby vaccination schedule was reduced in 2026, so not all vaccines are now recommended for all babies—knowing what’s still routine is crucial.
- Major differences exist between the CDC, WHO, and NHS schedules, which can confuse families, especially those moving between countries or states.
- Practical solutions include appointment reminders, evidence-based strategies for side effects, and knowing where to get help—especially for parents in high-risk or underserved groups.
- Understanding the Baby Vaccination Schedule: What Parents Need to Know
- How to Navigate and Stay on Track With Your Baby’s Vaccinations
- Advanced Analysis & Common Pitfalls (CDC vs WHO vs NHS)
- Conclusion
- Frequently Asked Questions
Understanding the Baby Vaccination Schedule: What Parents Need to Know
A baby vaccination schedule is a timetable recommending when your child should receive each vaccine to protect them from serious diseases. In 2026, the U.S. Department of Health and Human Services (HHS) drastically changed the baby vaccination schedule, removing several vaccines from the list recommended for all children. The updated approach focuses on 11 core diseases, moving others to “shared clinical decision-making” or “high-risk only.”
Internationally, different health systems still take broader approaches. The World Health Organization (WHO) and the UK NHS continue to recommend more vaccines for all babies, including hepatitis B at birth, rotavirus, and combinations like the 6-in-1 vaccine.
These changes can cause confusion for families—especially with many pediatricians now sticking to the American Academy of Pediatrics (AAP) guidelines, which remain broader than the official CDC schedule.

To ensure your baby is fully protected, it is crucial to:
- Know which vaccines are routine, which require personalized decisions, and which are only for high-risk babies
- Understand how global vaccine schedules differ—especially if you travel, relocate, or have a cross-border family
- Be proactive in getting clear, simple answers from your healthcare provider regarding their approach to vaccinations
For more on early child safety beyond vaccination, see our guide on safe sleep solutions.
How to Navigate and Stay on Track With Your Baby’s Vaccinations
Staying on track with your baby’s vaccination schedule is one of the best ways to prevent severe illness. Here’s a step-by-step process for parents navigating the new landscape in the U.S., with actionable advice for families worldwide.
- Get the latest schedule from your provider. Ask directly: “Are you following the CDC/HHS 2026 guidance or the AAP’s broader recommendations?” Save a copy for your records and clarify which category (routine, SCDM, high-risk) each vaccine now falls into.
- Book appointments in advance and use reminders. At every visit, pre-book the next one and sign up for text, email, or app reminders. Even in systems with well-organized clinics, missed appointments are a top reason for under-vaccination.
- Do not postpone for minor illnesses. Unless your baby has a high fever or is seriously unwell, stick to the vaccination timetable. Delaying for colds or teething is rarely necessary, yet common.
- Consolidate all vaccine records. Keep a single paper record (like the UK “Red Book”) or digital app up-to-date. Photograph your consolidate all vaccine records after each visit. If you move clinics or countries, bring every record with you and show it to your new doctor. Learn more about consolidating care and milestones in our milestone tracker guide.
- Address missed or delayed doses quickly. Vaccines can almost always be caught up—do not restart the entire series. Discuss catch-up options at your next visit, especially after moves or scheduling gaps.
- Discuss “non-routine” vaccines. Ask your provider if vaccines now under SCDM or “high-risk only” are recommended for your baby’s circumstances. This transparency avoids confusion over their value. For more on shared vaccine decisions, read this expert breakdown.
- Plan for normal side effects and know red flags. Most babies experience mild fever, fussiness, or redness at the injection site. Use mild fever, age-appropriate pain relievers as advised, keep your baby hydrated, and know when to seek urgent care for symptoms like facial swelling or persistent high fever. If you have worries about allergies or adverse events, consult your pediatrician—a referral to an immunization specialist may ease your concerns.
- Don’t let cost be a barrier. If you’re in the U.S. and concerned about vaccine costs, ask if your provider participates in the Vaccines for Children (VFC) program. Every country is different—tax-funded systems like the UK NHS provide all vaccines free at the point of care.
For a wider look at infant care essentials and keeping development on track, consider reading about baby care essentials.
Advanced Analysis & Common Pitfalls (CDC vs WHO vs NHS)
The recent overhaul to the CDC baby vaccination schedule has created both new opportunities and serious challenges for parents and providers alike. Here’s what to watch for—along with a point-by-point comparison for families navigating multiple systems.
- Vaccine type confusion: Some parents think “not routine” means “not recommended.” This is not always true—many vaccines that moved to “shared decision” or “high-risk only” are still highly beneficial for the majority of babies. For instance, the rotavirus and hepatitis B vaccines remain crucial in global recommendations. See external expert source.
- Delayed or missed doses: These remain highest among families with work constraints, transport barriers, or low health system engagement, especially when facing complex schedules. Single-parent households and those moving between care systems are most affected.
- Record fragmentation: Moving between providers, crossing borders, or losing paper records creates uncertainty about which vaccines have been received. This is especially challenging for migrant or refugee families.
- Cost/insurance issues: In the U.S., shifting vaccines out of the “routine” category sometimes triggers administrative hurdles, with parents unsure whether they’ll be covered under insurance or public programs like VFC. For UK parents, funding is stable, but for U.S. families, clarifying eligibility early helps avoid unexpected bills. More in-depth info can be found at the HHS source.
- Clinic/system-level barriers: Limited clinic hours, staff shortages, or vaccine stock-outs mean scheduling or walk-in options may not always be flexible enough for working parents.
| Vaccine | CDC (US, 2026) | WHO (Global) | NHS (UK, 2024) |
|---|---|---|---|
| DTaP/Tdap | Routine | Routine | Routine (6-in-1) |
| Hepatitis B | High-risk/newborns only | Routine (birth + series) | Routine (6-in-1, incl. birth doses) |
| Rotavirus | Shared decision-making | Routine (oral, infancy) | Routine |
| Pneumococcal | Routine | Routine | Routine |
| MMR | Routine | Routine (measles-containing) | Routine |
| Varicella | Routine | Depends (not routine everywhere) | Routine |
| Influenza | Shared decision-making | High-risk/optional | Not in baby schedule (age 2+) |
| MenB/MenACWY | Shared decision/high-risk | High-risk regions/groups | Routine (MenB early) |
See our companion allergy guide if you are concerned about vaccine reactions or have a baby with a complex medical history.
Overlooked problems:
Many resources blame missed shots on “parent forgetfulness,” but system-level issues—like short clinic hours or language barriers—play a huge role. Likewise, articles rarely address the impact of schedule cuts on disadvantaged families or the challenge of reconciling vaccine histories for children born abroad or in refugee circumstances.

Conclusion
Keeping up with the right baby vaccination schedule is becoming more complex, especially in the U.S., where recent changes create differences between pediatricians and official recommendations. To give your child the best protection, stay well-informed, use proactive scheduling strategies, and never hesitate to ask your provider about any updates or concerns.
Take action today: review your baby’s vaccine record, clarify your pediatrician’s approach, and schedule any needed appointments. For more parenting topics, browse our guides on developmental milestones and baby care tips.
Frequently Asked Questions
What are the biggest changes to the U.S. baby vaccination schedule in 2026?
The CDC/HHS schedule now only recommends 11 vaccines routinely for all children, moving others like hepatitis B (except high-risk newborns), rotavirus, and influenza to “shared clinical decision-making.” Many pediatricians continue to use the older, broader schedule from the American Academy of Pediatrics.
If my baby was born abroad, how can I catch up to my local vaccination schedule?
Bring all available paper and digital records. Your pediatrician can use global comparison charts to see what matches up, and develop a catch-up plan—most doses do not need to be restarted. For more advice, see baby milestone tracking.
What should I do if my clinic is out of a certain vaccine?
Use equivalent brands if available and appropriate, and follow national catch-up guidance. Don’t delay the entire series. Ask about other local clinics or the possibility of temporary substitutions.
Will insurance or Medicaid always cover my baby’s vaccines?
Not always. The Vaccines for Children (VFC) program covers many recommended vaccines without cost if your family qualifies. However, insurance confusion is rising for vaccines no longer listed as “routine,” so clarify coverage with your provider in advance. If cost is an issue, ask your public health department about no-cost options.
Is it safe to vaccinate my baby if they have a cold?
Yes—unless your baby has a high fever or is very unwell, minor illnesses aren’t a reason to delay vaccinations. Prompt vaccination keeps your schedule on track and reduces risk of disease.
—